Nineteen-year-old Angelina Benson clung to the back of a motorbike as labor pains intensified, traveling miles from her village after spending hours at a local clinic that could not manage her condition.
“They kept me there, but the pain continued,” she said. “Then they told me to go to the hospital.”
By the time she reached Wau Teaching Hospital, she was in distress and rushed into surgery within minutes of arrival.
“They gave me good medical support,” she said, cradling her newborn. “Now I feel fine.”
Her journey reflects a broader reality across South Sudan, where delays in accessing skilled care remain a major risk for mothers, even as improvements inside hospitals begin to change outcomes.
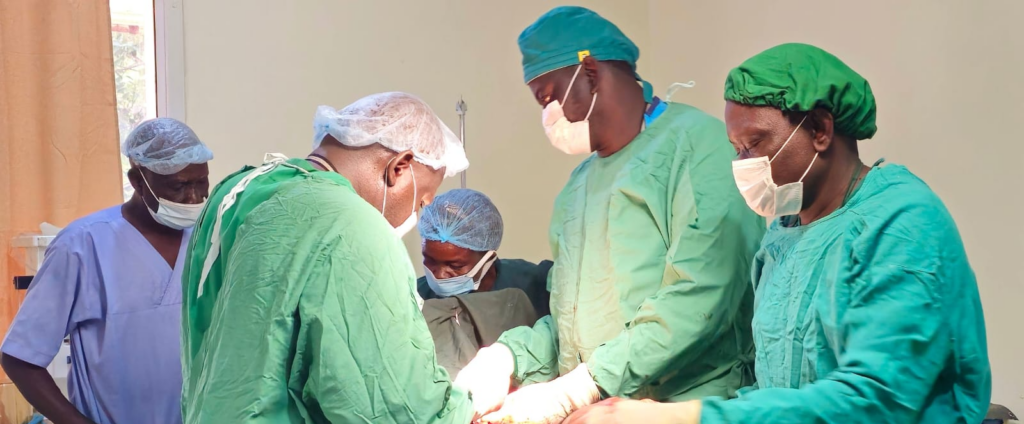
At Wau Teaching Hospital, one of the main referral facilities in the Greater Bahr el Ghazal region, midwives say recent training supported by UNICEF is helping them manage complications that once proved fatal.
“You must make sure the mother and the baby are safe before and after delivery,” said Adim Deng Deng, a registered midwife with six years of experience. “Sometimes you work the whole night without sleeping.”
Deng is among a growing number of male midwives in the country, a shift that is challenging traditional perceptions of maternal care. Inspired by his mother, a traditional birth attendant, he chose the profession to improve how women are treated during childbirth.
“I saw many mothers suffer from infection and bleeding,” he said. “Now we know how to prevent that and save lives.”
In recent years, staff at the hospital have undergone emergency obstetric care training supported by UNICEF under the Health Sector Transformation Project, as well as programs backed by partners including CORDAID, the World Health Organization, the United Nations Population Fund and the Red Cross.
The training focuses on managing complications such as obstructed labor, preventing infections and performing assisted deliveries.
“It improved the quality of care,” Deng said. “It renews our knowledge and gives us updates on how to treat mothers and newborns.”
He cited practical skills now used daily, from infection prevention and control to assisted vaginal delivery and managing complications after miscarriage.
Across the maternity ward, the impact is visible not only in outcomes but also in patient experience.
“When a mother comes in pain, you must be close to her and understand her,” said midwife James Ambrose. “That helps her a lot.”
Deng said attitudes toward male midwives are gradually changing.
“Some people think this is women’s work, but that is not true,” he said. “Many mothers prefer male midwives because we handle them gently and with care.”
Patients say the difference is noticeable.
Fatima Moussa, a 26-year-old Sudanese refugee, described a long day in labor before safely delivering her first child at the hospital.
“The services are good,” she said. “They treated me well. I felt safe.”
Hospital director Dr. Bulus Lawrence Ndenge said improvements are linked to both training and stronger coordination across facilities.
“Previously, many complications came from peripheral centers where staff could not detect danger signs early,” he said. “Now they are managing better and referring earlier.”
The hospital records between 120 and 170 deliveries per month, including cesarean sections, and serves a population of hundreds of thousands.
According to Ndenge, early 2025 figures show a decline in maternal deaths within the facility.
“In the first months of the year, we recorded very few maternal deaths, and currently none,” he said.
Still, he warned that the progress remains fragile.
Funding delays under the Health Sector Transformation Project have disrupted payments to health workers, with some going months without incentives.
“Most of us are facing financial challenges,” Deng said. “Our incentives are delayed for five or even six months. It discourages staff.”
The maternity department has around 26 midwives covering multiple units, far from enough for the patient load. On a typical day, more than 20 women arrive to deliver, stretching already thin teams.
Outside the hospital, access to care remains a critical barrier.
Many women, like Angelina, first seek help at smaller clinics or attempt home deliveries before being referred, often too late. Transport is limited, with only a handful of ambulances serving large areas.
Deng recalled a case that still troubles him.
“A mother came after attempting to deliver at home,” he said. “The uterus ruptured and the baby died. It was very heartbreaking.”
Across South Sudan, funding constraints have already reduced support to some health facilities, affecting staffing, supplies and outreach services.
Health experts warn that while training is improving care inside facilities, broader systemic challenges from transport to staffing continue to put lives at risk.
Back in the maternity ward in Wau, Angelina rests beside her newborn, her journey ending safely but only after a race against time.
For midwives like Deng, each life saved underscores both the progress made and the challenges that remain.
In a country where safer births increasingly depend on trained hands, the gains are real, but the system delivering them remains fragile.






 and then
and then